Best Diabetic Retinopathy Treatment: When to Start and What to Expect
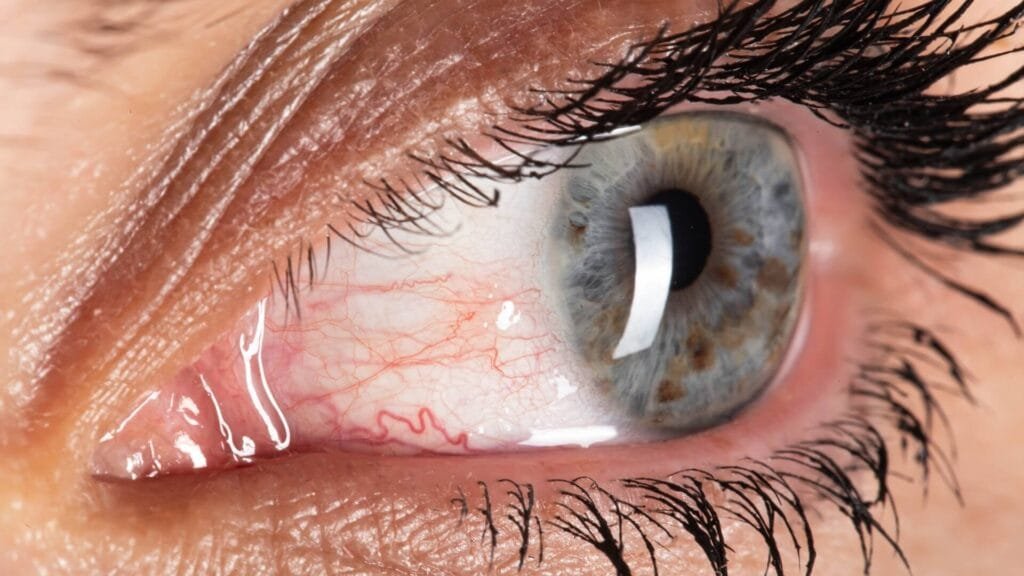
People living with diabetes often focus on managing blood sugar, but regular eye care is equally important for protecting long-term vision. Diabetic retinopathy develops when high blood sugar damages the tiny blood vessels in the retina, the light-sensitive tissue responsible for clear vision. Over time, these vessels may leak, weaken, or become blocked, gradually affecting sight. Hearing about diabetic retinopathy may raise concerns like, “Will this affect my vision?” The reassuring news is that with regular eye exams and the best diabetic retinopathy treatment can effectively manage the most diabetes-related vision problems. Treatment decisions depend on the stages of diabetic retinopathy and detailed retinal findings. At Aarya Eye Care, specialists use advanced retinal diagnostics and stage-based treatment to protect long-term vision.
What Is Diabetic Retinopathy?
Diabetic retinopathy is a progressive retinal disorder caused by long-term damage to the blood vessels of the retina. Elevated blood glucose levels weaken these vessels, leading to leakage, blockage, or abnormal blood vessel growth (neovascularization).
Doctors classify the disease into different stages of diabetic retinopathy, which help determine suitable diabetic retinopathy treatment options. The condition is broadly divided into two stages:
- Non-proliferative diabetic retinopathy (NPDR) – early stage with vessel damage
- Proliferative diabetic retinopathy (PDR) – advanced stage with abnormal vessel growth
A common complication is macular edema, where fluid builds up in the macula and causes vision problems. Because the condition often develops slowly without early symptoms, regular eye examinations are important for early detection.
Understanding the Stages of Diabetic Retinopathy
Mild Non-Proliferative Diabetic Retinopathy (NPDR)
This is the earliest stage of diabetic retinopathy. Small swellings called microaneurysms form in retinal blood vessels. Most patients have no symptoms, so doctors usually recommend monitoring to decide when to treat diabetic retinopathy.
Moderate NPDR
At this stage, some retinal blood vessels leak or become blocked. Mild retinal swelling may occur. Doctors evaluate scans to determine appropriate diabetic retinopathy treatment options.
Severe NPDR
Several retinal vessels become blocked, reducing oxygen supply to the retina. This increases the risk of disease progression, and doctors may recommend laser treatment for diabetic retinopathy.
Proliferative Diabetic Retinopathy (PDR)
This advanced stage involves abnormal blood vessel growth on the retina. These fragile vessels may bleed and threaten vision. The best diabetic retinopathy treatment may include injections, laser therapy, or surgery.
Diabetic Macular Edema (DME)
Macular edema occurs when fluid builds up in the macula, causing central retinal swelling. It can develop at any stage and is a common cause of vision loss in diabetic patients.
When to Treat Diabetic Retinopathy
Modern ophthalmology offers several diabetic retinopathy treatment options, depending on the severity of the condition.
Observation and Systemic Control
For early stages, doctors may recommend monitoring rather than active procedures. Key systemic management includes:
- Keeping HbA1c within a healthy range.
- Blood pressure control
- Cholesterol management
- Scheduled retinal examinations
Controlling systemic health factors significantly slows disease progression.
Anti-VEGF Eye Injections
Eye injections for diabetic retinopathy target a protein called VEGF (vascular endothelial growth factor), which promotes abnormal blood vessel growth and fluid leakage. Anti-VEGF medications reduce retinal swelling and prevent new vessel formation. Treatment often begins with monthly injections, gradually extending the interval based on response. The procedure is quick, typically taking only a few minutes under local anesthesia.
Steroid Injections
Steroid injections are sometimes used when retinal swelling persists despite other therapies. They help reduce inflammation and fluid accumulation in the retina. However, they may increase the risk of cataracts or elevated eye pressure, so careful monitoring is required.
Laser Treatment (Panretinal Photocoagulation)
Laser treatment for diabetic retinopathy is commonly used in proliferative disease. The laser creates small controlled burns in the peripheral retina, reducing oxygen demand and slowing abnormal blood vessel growth. This treatment is typically completed as an outpatient procedure and generally lasts under 30 minutes. Some patients may experience temporary blurred vision or mild discomfort.
Vitrectomy Surgery
Vitrectomy surgery is recommended in advanced cases, particularly when there is persistent bleeding inside the eye or retinal detachment. During this procedure, the surgeon removes the vitreous gel and replaces it with a clear solution, allowing better visualization and repair of the retina. Recovery may require special head positioning depending on the surgical technique.
What to Expect During Treatment
Before Treatment
Patients undergo detailed eye evaluation, including retinal imaging and dilation.
During Injection
The eye is numbed using anesthetic drops. The injection itself takes only a few seconds and causes minimal discomfort.
During Laser Treatment
Patients may see bright flashes of light. Mild discomfort is possible but usually manageable.
After Treatment
Temporary blurred vision is common. Follow-up visits help monitor healing and disease progression.
Can Diabetic Retinopathy Be Cured?
Diabetic retinopathy cannot be completely reversed once significant retinal damage has occurred. However, modern treatments can help control the disease and prevent severe vision loss. Early diagnosis and timely care play a key role in protecting long-term vision.
Seeking regular evaluation at the best eye care hospital in Thrissur can help detect retinal changes early and ensure appropriate treatment.
Risks of Delaying Treatment
Delaying treatment may lead to the complications, including:
- Retinal detachment
- Persistent retinal bleeding
- Advanced macular damage
- Permanent vision loss
Prompt treatment greatly improves the chances of preserving vision.
Prevention and Long-Term Management
Long-term prevention focuses on systemic health and regular eye monitoring.
Important preventive measures include:
- Keeping HbA1c within the recommended range
- Controlling blood pressure
- Dilated eye checkups once a year
- Healthy lifestyle habits
- Avoid smoking
Early detection remains the most effective strategy for preventing diabetes-related vision loss.
Frequently Asked Questions
Is laser treatment painful?
Laser therapy may cause mild discomfort but is generally well tolerated.
Can vision improve after treatment?
In many cases, treatment stabilizes vision and may lead to improvement if swelling decreases.
Does the treatment provide long-term results?
Diabetic retinopathy requires ongoing monitoring because the disease can progress over time.
How often should diabetics get eye exams?
Most diabetic patients should undergo a comprehensive dilated eye examination at least once a year.
Conclusion
Diabetic retinopathy is an eye condition associated with diabetes, but it can be effectively managed with proper care. Understanding the stages of diabetic retinopathy and knowing when to treat diabetic retinopathy are essential for protecting long-term vision. With best diabetic retinopathy treatment options, including injections, laser therapy and surgery, most vision loss can be prevented when treatment begins at the appropriate stage. Regular retinal screening and early intervention play a crucial role in preserving eyesight. Patients seeking specialized retinal care can consult experts at Aarya Eye Care, widely recognized as a best eye hospital in Thrissur, for comprehensive evaluation and advanced treatment of diabetic eye diseases.