Keratoconus: Early Signs, Causes, and the Right Time to Start Treatment
Have you heard about keratoconus, a condition that often begins with subtle symptoms like frequent changes in glasses power, mild blur, or reduced clarity at night? These changes are often treated as normal and are commonly linked to general blurred vision causes, leading many people to simply update their prescriptions. However, such patterns may point to keratoconus early signs rather than routine vision changes. Keratoconus progresses gradually by altering the shape of the cornea, leading to increasing visual distortion over time. When identified early, it can be managed effectively, while delays can make treatment more complex. This guide provides a clear understanding of keratoconus, helping you recognise early signs and take timely, informed action. If you are noticing these changes, consulting the best eye hospital in Thrissur can help ensure accurate diagnosis and appropriate care at the right stage.
What Is Keratoconus?
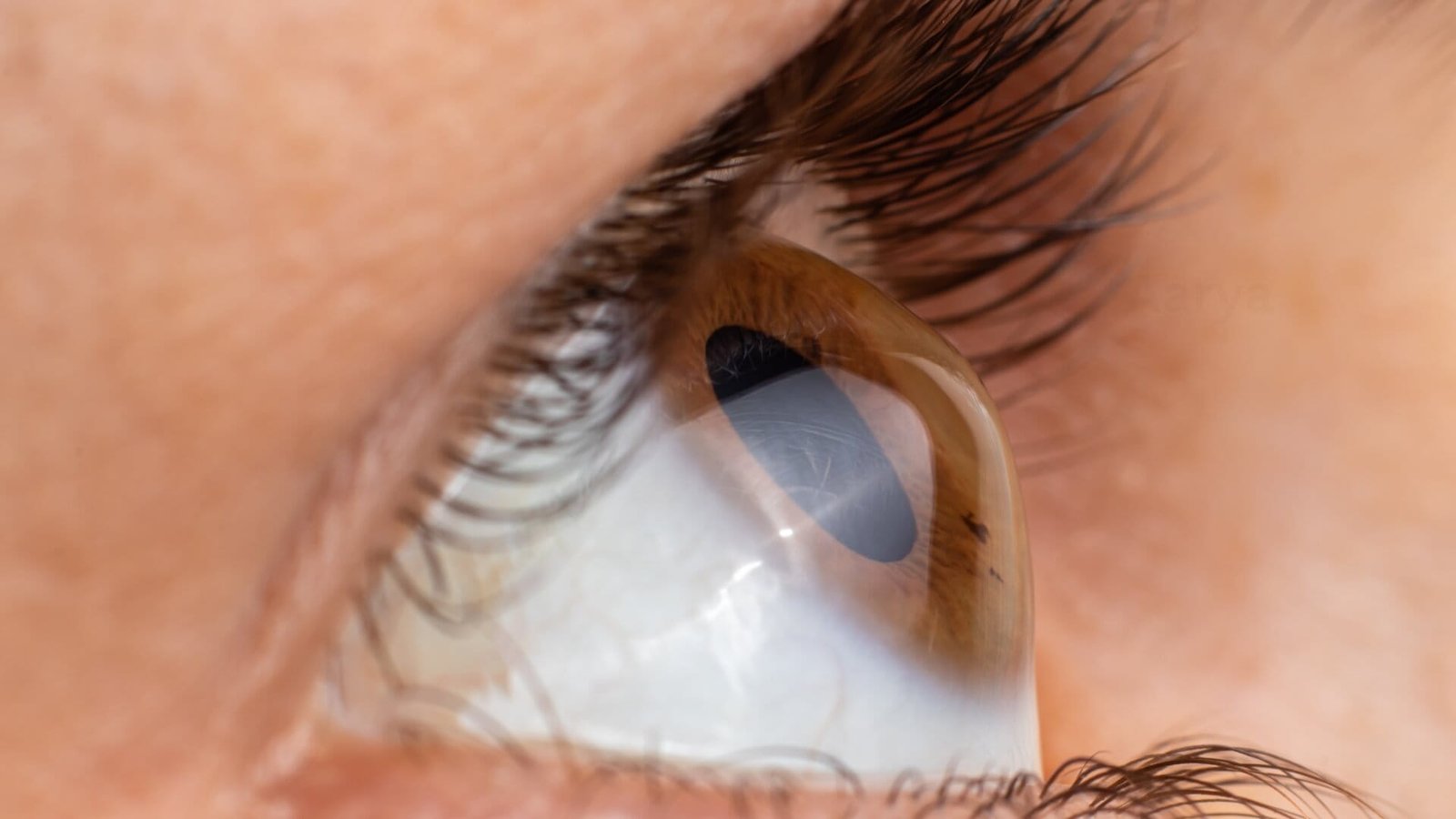
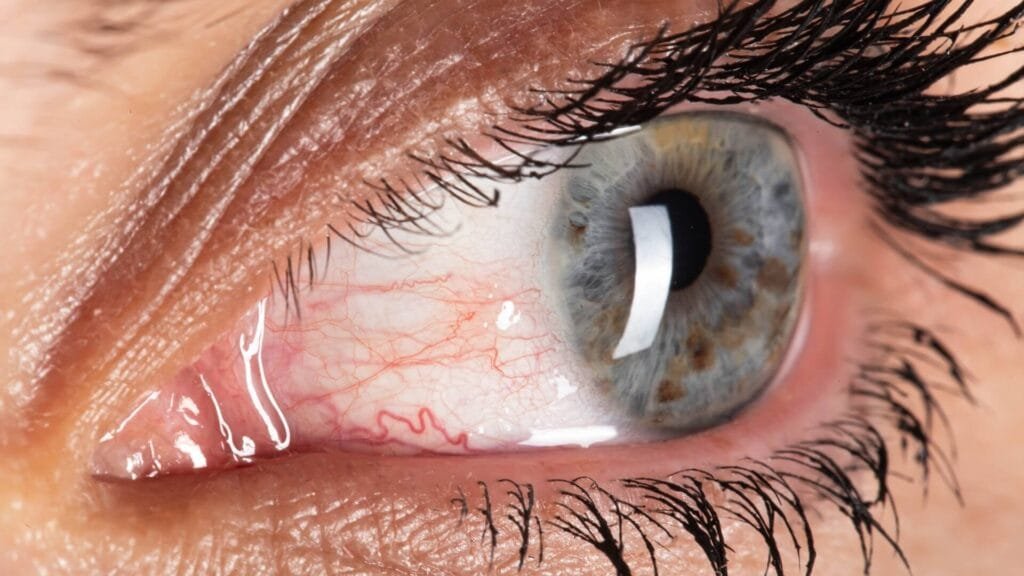
Keratoconus is a corneal thinning disease in which the normally round cornea gradually weakens and bulges outward into a cone shape. This structural change disrupts how light enters the eye. Instead of focusing cleanly on the retina, light scatters irregularly, leading to irregular astigmatism and distorted vision. This defines the keratoconus meaning, where vision becomes uneven and less predictable.
In simple terms:
- Normal cornea = smooth surface, resulting in clear vision
- Keratoconus cornea = uneven surface, leading to distorted and unstable vision
Keratoconus is not a static condition. It progresses over time, often silently in the early stages, making early understanding and detection essential.
Early Signs of Keratoconus
Recognising early symptoms of keratoconus is critical because this is the window where intervention is most effective.
Common Symptoms and Why They Happen
- Frequent prescription changes
The cornea keeps changing shape, so glasses power does not remain stable. - Blurred or distorted vision
Irregular corneal curvature causes uneven light refraction. - Ghost vision (double or shadow images)
Light splits into multiple focal points due to corneal irregularity. - Glare and halos around lights
Scattered light increases sensitivity, especially at night. - Poor night vision
Larger pupil size in low light exposes more corneal irregularities. - Eye strain and headaches
Constant visual correction effort fatigues the eyes.
When to Seek Medical Attention?
If you notice frequent changes in glasses power combined with night vision issues or ghosting, it is no longer routine. It requires evaluation.
Causes of Keratoconus
Keratoconus does not have a single trigger. It develops due to a combination of biological and behavioral factors. Let’s check keratoconus risk factors.
Genetics
There is a clear hereditary link. If a family member has keratoconus, the risk increases significantly. However, not all cases are inherited.
Eye Rubbing (Critical Factor)
This is one of the most underestimated but high-impact causes.
Repeated eye rubbing:
- Weakens corneal structure
- Increases mechanical stress
- Accelerates progression
This is not a minor habit. It is a direct risk multiplier.
Allergies
Chronic eye allergies lead to itching, which leads to rubbing, creating a cycle that worsens corneal damage.
Weak Corneal Structure
At a micro level, keratoconus is linked to weakened collagen fibers in the cornea. This reduces its ability to maintain shape under normal pressure.
How Keratoconus Progresses
Understanding keratoconus progression is essential because the condition develops gradually and each stage impacts vision differently. Recognising these keratoconus stages early helps in making timely treatment decisions.
Early Stage
- Mild distortion in vision
- Slight blur or frequent changes in glasses power
- Glasses or soft contact lenses still provide good correction
At this stage, the cornea has just begun to weaken and change shape. The symptoms are subtle, which is why they are often overlooked or mistaken for routine refractive changes.
Risk if ignored:
Progression continues silently and the underlying structural changes remain unaddressed.
Moderate Stage
- Increasing irregular astigmatism
- Glasses no longer provide clear or stable vision
- Specialised lenses such as RGP or scleral lenses become necessary
Here, the corneal shape becomes more uneven, leading to noticeable visual distortion. Patients may experience ghosting, glare or difficulty with night vision.
Risk if ignored:
Corneal instability increases, making vision correction more challenging and reducing the effectiveness of non-invasive options.
Advanced Stage
- Significant corneal thinning and possible scarring
- Severe visual distortion and reduced clarity
- High dependence on specialised lenses or surgical options
At this stage, the cornea becomes highly irregular and vision may not be adequately corrected even with lenses. In certain cases, surgery may be needed.
Risk if ignored:
Permanent vision compromise, with increased likelihood of requiring advanced keratoconus treatment such as corneal transplant.
When Should You Start Treatment?
A common misconception is waiting until keratoconus worsens before starting treatment, whereas early intervention is more effective.
Start treatment when:
- Diagnosis is confirmed
Once keratoconus is identified through proper evaluation, it is important to act early rather than monitor passively. Early confirmation gives you the opportunity to stabilize the condition before significant changes occur. - Corneal topography shows progression
Even if your vision feels stable, changes in corneal shape detected through a corneal topography test can indicate progression. Treatment decisions are often based on these structural changes, not just symptoms. - Vision becomes unstable
If you notice frequent prescription changes, inconsistent clarity, or difficulty achieving sharp vision even with correction, it suggests that the cornea is continuing to change.
Why early treatment matters
- Less invasive
Early keratoconus treatments like corneal cross-linking are simpler and focus on stopping progression before structural damage increases. - More cost-effective
Managing keratoconus early helps avoid the need for multiple interventions or advanced procedures later. - More predictable outcomes
Early intervention is highly effective in stabilising the condition and preserving long-term vision quality.
Diagnosis of Keratoconus
Diagnosing keratoconus early is important because the initial changes in the cornea can be subtle and easily missed during routine eye tests. A more detailed keratoconus diagnosis test is often required to identify these early structural changes.
Key Diagnostic Tools
- Corneal Topography
This test maps the shape of the cornea and helps detect even small irregularities. It is one of the most reliable ways to identify keratoconus at an early stage. Access to accurate corneal topography in Thrissur can make a significant difference in early detection. - Advanced Imaging Systems
These scans assess corneal thickness and structure, helping specialists confirm the diagnosis and monitor progression over time.
Why Accurate Diagnosis Matters
- Helps detect the condition early
- Supports timely treatment decisions
- Reduces the risk of progression
Not all clinics are equipped to detect early keratoconus. Choosing the best eye hospital in Thrissur ensures access to the right technology and expertise for accurate diagnosis and effective management.
Treatment Options for Keratoconus
Treatment for keratoconus focuses on two key goals, stopping progression and improving vision. The approach depends on the stage of the condition.
Corneal Collagen Cross-Linking (CXL)
Corneal cross linking treatment is one of the most effective options to control keratoconus progression.
- Strengthens corneal collagen fibres
- Helps stop further thinning and bulging
- Most effective when done in the early stages
Often referred to as CXL surgery for keratoconus, this treatment is widely recommended as a primary option in keratoconus treatment at an early stage.
Outcome: stabilisation of the condition and prevention of further deterioration
Contact Lenses for Keratoconus
Specialised keratoconus contact lenses are used to improve visual clarity by creating a smooth optical surface.
- RGP (Rigid Gas Permeable) lenses provide sharper vision
- Scleral lenses for keratoconus offer better comfort and stability in advanced irregularity
It is important to note that while these lenses improve vision, they do not stop the progression of keratoconus.
Intacs / Corneal Implants
Intacs for keratoconus, also known as corneal ring implants, are small segments inserted into the cornea.
- Help reshape the cornea
- Improve visual quality
- Suitable for moderate stages where lenses are insufficient
This option can delay or reduce the need for more invasive procedures.
Corneal Transplant
In advanced cases, keratoconus surgery may involve a corneal transplant for keratoconus.
- Considered when there is severe thinning or scarring
- Involves replacing the damaged cornea with donor tissue
This is typically the last-line treatment when other options are no longer effective.
Why Early Treatment Matters
The timing of treatment directly impacts outcomes. Early intervention offers clear advantages compared to delayed management.
Early Stage
- Simple procedures like CXL
- Lower treatment cost
- Better and more stable visual outcomes
Delayed Stage
- Multiple and more complex interventions
- Increased overall cost
- Higher likelihood of surgical procedures
Understanding the benefits of early keratoconus treatment is key, as timely care helps prevent keratoconus progression and preserves long-term vision quality.
Why Choose Aarya Eye Care
Aarya Eye Care follows a structured and precision-driven approach to managing keratoconus, with a strong focus on early detection and stage-based treatment. The centre is equipped with advanced corneal imaging systems that enable accurate and early diagnosis, which is critical in identifying subtle changes before the condition progresses. With dedicated expertise in diagnosing and managing complex corneal conditions, the clinical approach is personalized to each patient through step-by-step treatment planning based on the stage of keratoconus. This ensures that every intervention is timely, appropriate and aligned with long-term visual stability. For those searching for the best eye hospital in Thrissur for reliable keratoconus treatment Thrissur, the focus should go beyond basic care. It should include access to advanced diagnostics, structured management and guidance from an experienced eye specialist Thrissur, all of which are central to effective keratoconus care.
Frequenlty Asked Questions
Can keratoconus be cured?
No. It can be managed and stabilised, especially with early treatment like CXL. The focus of treatment is to stop progression and maintain the best possible vision over time.
Is keratoconus hereditary?
Yes, genetics can play a role, though not all cases are inherited. If there is a family history, regular eye check-ups can help in early detection.
Is CXL painful?
It is typically performed under anaesthesia. Mild discomfort may occur during recovery. Most patients are able to return to normal activities within a few days with proper care.
Can I use my mobile or watch TV with keratoconus?
Yes, but unmanaged strain and dryness should be avoided. Using proper vision correction and taking regular breaks can help maintain comfort.
How fast does keratoconus progress?
Progression varies. In younger individuals, it can advance rapidly, making early detection critical. Regular monitoring helps track changes and guide timely treatment decisions.